Español
Tick-borne diseases, such as Lyme disease, are on the rise in people & dogs. Reported cases in people in the U.S. increased from about 12,000 annually in 1995 to approximately 35,000 in 2019, according to the Centers for Disease Control & Prevention. However, not all diagnosed cases are reported & the CDC believes the true number of human infections is likely closer to 476,000 per year.
The U.S. Food & Drug Administration regulates products that are used to help prevent, diagnose, & treat this complex disease.
Who Gets Lyme Disease, What Time of Year?
Lyme disease is a bacterial infection most commonly transmitted via the bite of infected ticks, which attach to any part of the body.
The CDC recommends you check your dog daily, especially after they spend time outdoors. Pay particular attention to the collar area & around the eyelids, ears, tail, under the front legs, & between the back legs & toes.
On people, you will most often find ticks in moist or hairy areas such as the groin, armpits, scalp, & other hard-to-see areas of the body. & while everyone is susceptible to tick bites, campers, hikers, & people who work in gardens & other woody, & brushy areas with high grass & leaf litter, are at the greatest risk of tick bites. As many a suburban gardener can attest, with the expansion of the suburbs & a push to conserve wooded areas, deer populations are thriving. Deer are important sources of blood for ticks & are important to tick survival & movement to new areas, increasing the contact between people & ticks that carry the bacteria. Read more about the lifecycle of the bacteria & how it is transmitted to people & dogs.
In most cases, a tick must be attached for 36 to 48 hours or more before the Lyme disease bacterium can be transmitted. If you remove it within 24 hours, the risk is greatly reduced. Symptoms of Lyme disease may take 3-30 days or longer to appear.
In the majority of cases, tick bites are reported in the summer months when ticks are most active & people spend more time outdoors. But this can extend into the warmer months of early autumn, or even late winter if temperatures are unusually high. Similarly, a mild winter can allow ticks & other insects to thrive & emerge earlier than usual.
How to Safely Remove a Tick
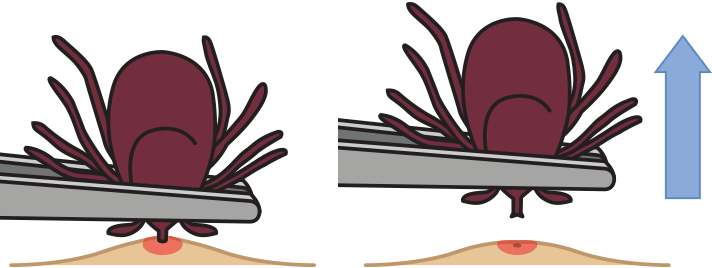
- Using fine-tipped tweezers, grasp the tick as close to the skin’s surface as possible.
- Pull upward with steady, even pressure. Don’t twist or jerk the tick. Your goal is to remove the entire tick, ideally in one piece, including the mouth parts embedded under the skin.
- Thoroughly clean the bite area & your hands with rubbing alcohol, an iodine scrub, or soap & water.
Not all ticks carry Lyme disease, & some ticks carry other diseases. To avoid infecting yourself, never crush a tick with your fingers. For more information on the safe removal, disposal & identification of ticks visit CDC.gov/ticks.
Lyme Disease in People
Prevention
What can I do to prevent Lyme disease?
- Avoid wooded, brushy, & grassy areas, especially during warmer months (April – September), although tick exposure can occur anytime.
- Wear light-colored clothing so that you can see ticks that get on you.
- Treat clothing & gear with products containing 0.5% permethrin.
- Apply insect repellents on uncovered skin, & ensure the products are registered by the Environmental Protection Agency.
- Wear long pants & long-sleeved shirts, & shoes that cover the entire foot.
- Tuck pant legs into socks or shoes, & tuck shirts into pants.
- Wear a hat for extra protection.
- Walk in the center of trails to avoid brush & grass.
- Remove your clothing after being outdoors, & wash & dry them at high temperatures.
- Do a careful body check for ticks after outdoor activities.
There are no licensed vaccines available in the U.S. to aid in the prevention of Lyme disease in people.
Symptoms & Stages
Symptoms of early-stage Lyme disease include:
- muscle & joint aches
- headache
- fever
- chills
- fatigue
- swollen lymph nodes
Another common symptom of Lyme disease is a rash (referred to as “Erythema migrans”). As many as 80% of infected people may develop a rash, however the characteristic “bull’s-eye” rash appears only 20% of the time.
Later-stage symptoms may not appear until weeks or months after a tick bite. They include:
- irregular heartbeat &/or heart palpitations
- arthritis (usually seen as pain & swelling in large joints, especially the knee)
- nervous system abnormalities
When left untreated, the bacterial infection can spread to joints, the heart, & the nervous system & cause permanent damage. Lyme disease is rarely fatal.
However, if not treated properly, Lyme disease can become a chronic illness where symptoms might continue for weeks, months, or even years after the initial tick bite.
Lyme Disease in Dogs
Dogs can get Lyme disease, too. Typical symptoms in dogs include swollen joints & lameness, fever, & loss of appetite. Experts in the FDA’s Center for Veterinary Medicine say dogs with Lyme disease occasionally develop serious kidney disease that can be fatal.
There are ways you can reduce your dog’s risk for tick bites & Lyme disease, which also reduces the risk of infection for you.
- Regularly check your dog for ticks.
- Avoid allowing your dog to roam in tick-infested areas.
- Treat your dog year-round with topical, oral &/or collar tick products. Talk to your veterinarian about which product is best for your dog.
Lyme disease occurs much less frequently in cats than in dogs, & cats’ susceptibility to the disease continues to be the subject of research. However, the same precautions for dogs apply to cats, especially if your cat goes outside, because ticks on cats can be transferred to people & ticks carry other diseases besides Lyme disease that are harmful to cats.
There are several FDA-approved products that treat & control tick infestations. A couple of tick products are also approved in dogs to specifically prevent infections with the bacteria that causes Lyme disease by killing the ticks that carry the bacteria.
Lyme disease vaccines are available for dogs, but not for cats. Talk to your veterinarian to see if vaccination is appropriate for your dog.
Lyme Disease Tests & Treatment
If you think you or your dog may have Lyme disease, contact your physician or veterinarian right away.
Your doctor or veterinarian may test for Lyme disease, &/or they may immediately begin antibiotic treatment, depending on the symptoms you or your dog exhibit.
Most blood tests check for the antibodies produced by the body to fight Lyme disease. CDC experts report it may take several weeks after a tick bite for initial antibodies to develop. Because of this, the blood tests may not be accurate if done soon after a tick bite.
For this reason, your doctor or veterinarian may recommend treatment with antibiotics before the diagnostic tests are complete. According to the CDC & other experts, people treated with appropriate antibiotics in the early stages of Lyme disease usually recover rapidly & completely.
In dogs, the more subtle early stages of Lyme disease often go unnoticed. Even if your dog appears healthy, your veterinarian may recommend yearly screening for Lyme disease, especially if you live in an area where Lyme disease is common. If your dog’s blood test is positive, your veterinarian may recommend additional testing, such as a urinalysis.
Source: FDA Consumer Updates